- Home
- Applications
- Leukemia
ADC Development Services for Leukemia Research
Leukemia is the most common and lethal cancer in adults, and conventional therapies for this cancer have not shown meaningful changes for the past decades. As innovative next-generation immunotherapeutic agents, antibody-drug conjugates (ADCs) are being developed worldwide as a major strategy to combat cancer, and several ADCs have been approved for clinical use. With years of experience and high-end technologies in ADC development, Creative Biolabs has successfully developed a series of innovative and diversified ADC preparation platforms to provide fast and convenient services for our worldwide customers. Now we provide a full range of ADC design and construction service targeting the leukemia.
Introduction of Leukemia
Leukemia is a kind of blood cancer that usually begins in the bone marrow and the lymphatic system, which results in high numbers of abnormal blood cells called blasts or leukemia cells. The symptoms are characterized by bleeding, bruising, fatigued, fever, and an increased risk of infections due to a lack of normal blood cells. Currently, the specific cause of leukemia is unclear, the genetic factors and environmental factors are considered as the main reasons. Besides, some risk factors such as smoking, previous cancer treatment, genetic disorders, exposure to certain chemicals and family history of leukemia may cause leukemia. Generally, leukemia is divided into four main types including acute lymphoblastic leukemia (ALL), acute myeloid leukemia (AML), chronic lymphocytic leukemia (CLL) and chronic myeloid leukemia (CML).
About 90% of leukemias occur in adults, with AML and CLL being most common. However, about three-fourths of AML leukemia occurs in children. The diagnosises of leukemia include physical exam, blood tests and bone marrow test. Treatments for leukemia include chemotherapy, radiation therapy, biological therapy, targeted therapy, and stem cell transplant. Supportive care and palliative care also are required. The success of treatment relies on the type of leukemia and the age of the person. Commonly, if the individual is younger, which has a greater the average five-year survival rate.
Current Therapeutic Strategies for Leukemia
Treatment options for patients with leukemia have grown significantly beyond standard chemotherapy in recent years, especially some new targeted therapies such as the immunotherapy. Antibody-based therapies are the major advances, such as naked monoclonal antibodies, ADCs and bispecific T cell engaging (BiTE) antibodies, adoptive cellular therapies such as chimeric antigen receptor (CAR) T cells. Besides, other targeted therapies are being used in Philadelphia chromosome-positive (Ph+) ALL, Philadelphia-like (Ph-like) ALL, and T cell ALL.
As for the immunotherapy of ALL, CD20-targeted therapies include the Rituximab (A chimeric anti-CD20 monoclonal antibody), Ofatumumab and Obinutuzumab. CD22-targeted therapies include Inotuzumab ozogamicin (an ADC conjugated anti-CD22 monoclonal antibody to calicheamicin). CD19-targeted therapies include Blinatumomab, Chimeric antigen receptor (CAR) T cells, Denintuzumab (an ADC with a humanized anti- CD19 antibody conjugated to a microtubule-disrupting agent monomethyl auristatin F). During the treatment of Philadelphia chromosome-positive ALL, the main targeted treatment options are some tyrosine kinase inhibitors (TKIs) targeting the BCR-ABL tyrosine kinase including Imatinib, Dasatinib and Nilotinib, Ponatinib and ABL001 (Asciminib). In addition, NOTCH inhibitors are being used in the treatment of patients with relapsed and refractory T ALL.
Also, there are various targeted therapies for patients with CLL, including effective oral targeted therapies (such as ibrutinib, idelalisib, and venetoclax), and next-generation anti-CD20 monoclonal antibodies (such as obinutuzumab). These agents have resulted in improved outcomes in CLL, and each of these treatments is associated with a unique toxicity profile. In addition, a CD37-targeted antibody-drug conjugate IMGN529 is highly active against human CLL and presents significant potential in the CLL treatment.
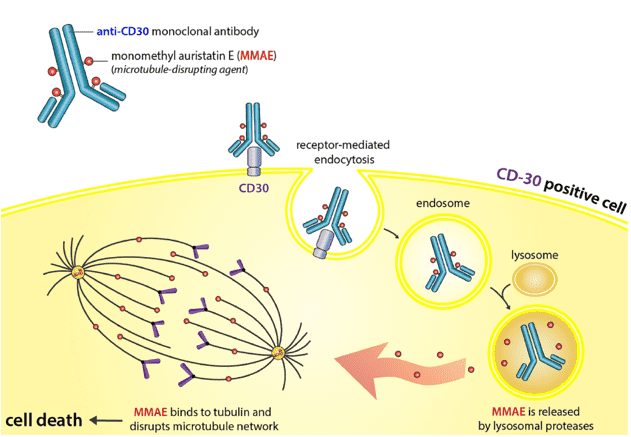 Fig.1 The mechanism of action of brentuximab vedotin.1,2
Fig.1 The mechanism of action of brentuximab vedotin.1,2
What Can We Do for You?
Although conventional therapies have shown some success in the treatment of cancer, they are often accompanied by severe side-effects due to the lack of target specificity. To overcome this flaw and improve the efficacy and safety of cancer treatment, targeted cancer therapies, especially ADCs, have been exploited actively and they are achieving a significant amount of attention during the recent years. With years of experience in antibody discovery and bio-conjugation field, Creative Biolabs is dedicated to helping our clients design and prepare highly customized ADCs targeting the leukemia using our featured services. Our ADC development services for the leukemia treatment include:
- ADC Development for AML
- ADC Development for Acute Lymphoblastic Leukemia ALL
- ADC Development for Chronic Lymphocytic Leukemia CLL
Creative Biolabs provides customized ADC development services targeting leukemia based on the advanced technology platform. Our professional scientists have extensive experience in antibody production, drug-linker complexes preparation and bio-conjugation. We are committed to providing high-quality ADCs construction services to promote the development of innovative cancer treatments. If you are interested in our service, please do not hesitate to contact us for more details.
References
- Iżykowska, Katarzyna, et al. "Novel targeted therapies of T cell lymphomas." Journal of hematology & oncology 13 (2020): 1-38.
- Distributed under Open Access License CC BY 4.0, without modification.
For Research Use Only. NOT FOR CLINICAL USE.

Online Inquiry
Welcome! For price inquiries, please feel free to contact us through the form on the left side. We will get back to you as soon as possible.
