Scientists have been hugely successful in developing a new type of anti-cancer therapy, immunotherapy, over the past decade, a treatment that attacks cancer cells by activating the body’s autoimmune system. One of the immunotherapies, called chimeric antigen receptor (CAR) T cell therapy, has achieved gratifying results in some cancer patients. Two CAR T-cell therapies (Kymriah and Yescarta) have been approved by the FDA in the United States for the treatment of acute lymphoblastic leukemia and large B-cell lymphoma.
Despite such great success, scientists still do not fully understand the mechanism by which CAR T cells function. A new study by researchers at the Moffet Cancer Research Center recently solved the problem and elucidated the specific mechanism by which CAR T cells play a role. the results were recently published in the journal Science Signaling.
CAR T cell therapy is a unique immunotherapy because it is made up of the patient’s own immune cells, which are collected and isolated from the patient’s blood. The collected T cells were then sent to the lab for modification, and the researchers added a special receptor called CAR to the T cells to identify cancer cells. These genetically engineered T cells are cultured and proliferated in the laboratory and eventually sent to the hospital for injection.
T-cell mutated genes have been optimized by several research groups to achieve the best anticancer immune response. One of the genes inserted into T cells is part of a T cell receptor (CD3 Zeta). In addition, other costimulatory molecules are included, and the latest third-generation CAR also includes a number of costimulatory molecular receptors. However, some studies have shown that the embedding of multiple costimulatory molecular receptors does not enhance the efficacy of the third generation of CAR T. In addition, other modifications focus on the structural design of the receptor, such as binding the receptor to the region of the cell. But so far, researchers do not know how these different genes and structural designs will affect biological signals and immune cell effects.
Given the growing use of CAR T-cell therapies, Moffet’s researchers believe it is important to understand the specific mechanisms by which these therapies work in patients. In order to better understand how CAR T cells work, A multidisciplinary team from Moffet used a series of proteomics-based techniques to compare CAR T cells that target the same molecules on cancer cells but have different intracellular design and anticancer activities. The researchers found that second-and third-generation receptors can bind to a range of molecules, some of which even have the opposite function. Importantly, only the second generation of CARs can stimulate expression similar to the natural version of CD3 Zeta. The researchers found that this activity of the second-generation receptors depends on the structural design of the intracellular region and has nothing to do with the structure of the costimulatory molecular receptor or binding region. In addition, through detailed phosphoproteomic analysis, the researchers found that the second-generation receptors activated downstream signaling molecules more effectively than the third-generation receptors.
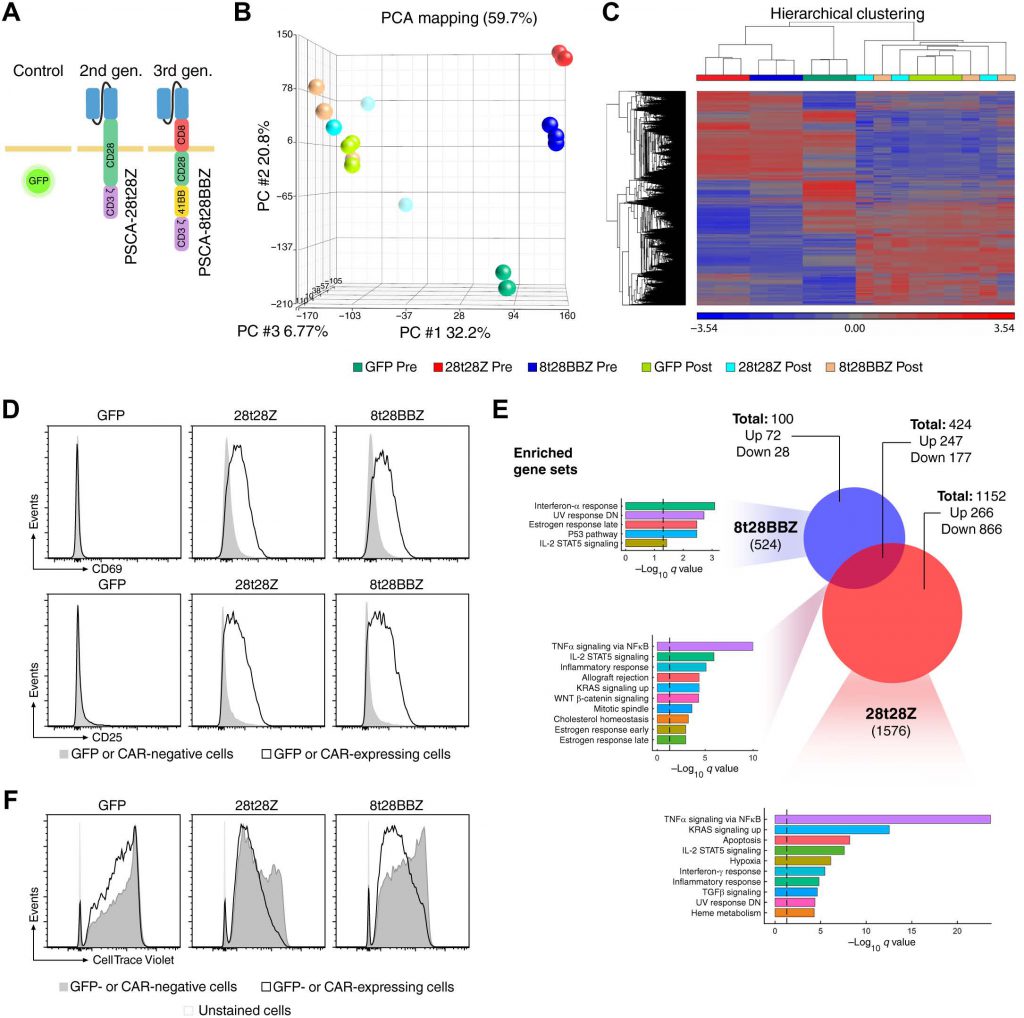
“These results suggest that the second generation of CARs can activate CD3 signals from other sources, which may lead to stronger signals and more effective anticancer effects. “Dr. Daniel Abate-Daga, an associate professor at the Moffet Department of Immunology who led the study, said. The team hopes their research will give researchers a better understanding of CARs, thereby improving the design and anticancer activity of CAR. By systematically analyzing the signal proteins interacting with CARs and the signaling pathways activated by different CARs structures, researchers can provide new tools for developing new receptors with more controllable functions.
“In our clinical use of these synthetic immunological products, this data may help design the next generation of CARs and combination therapies. “the lead author of the article, Dr. Maria Ramello, a postdoctoral researcher at Moffet, said.
Reference
Ramello, Maria C., et al. “An immunoproteomic approach to characterize the CAR interactome and signalosome.” Science signaling 12.568 (2019): eaap9777.
