What is Diabetes?
Diabetes is a metabolic disease, which is characterized by patients' blood sugar higher than the standard value for a long time. High blood sugar can cause symptoms commonly known as "three more, one less": overeating, overeating, polyuria, and weight loss. For type 1 diabetes, the symptoms will appear in a week to a month, while for type 2 diabetes, the symptoms will appear later. No matter what kind of diabetes, if not treated, it may cause many complications. The acute complications included diabetes ketoacidemia and hyperosmolality hyperglycemia non ketoacidosis coma; Serious long-term complications include cardiovascular disease, stroke, chronic kidney disease, diabetes foot, and retinopathy; Among them, diabetes is closely associated with heart failure and chronic kidney disease. Pancreatic islet transplantation has become a promising method to control blood sugar and reduce complications associated with diabetes. However, its clinical application is limited by many challenges, including the scarcity of donor islets, the risk of immune rejection, and complications related to existing transplantation procedures. These limitations have prompted people to explore alternative strategies for generating functional islets in vitro.
Islet Organoid as a Promising Model for Diabetes
Organoids are a cutting-edge technology that provides new models for developmental biology and disease research. Organoids are three-dimensional (3D) cultures derived from stem cells (pluripotent stem cells (PSCs) or organ restricted adult stem cells (ASCs) that can simulate specific organ functions. Compared to animal models, organoids can come from humans, thus avoiding inferring the findings of model animals to human needs; Compared to organ models directly derived from humans, organoids are easier to obtain and can be personalized. In clinical applications, organoids can serve as personalized high-throughput drug screening platforms for evaluating potential therapeutic effects and have the potential to become a new source of organ transplantation due to their functionality. However, the current organoid system has many problems, including limited cell composition, insufficient maturity, incomplete function, and low degree of vascularization. Because islets are closely related to the occurrence and development of diabetes, islet organs have attracted more and more attention. Pancreatic beta cells are considered the most basic component of the pancreas; therefore, previous studies have focused more on the generation of beta cells from stem cells, namely stem cell-derived beta cells (sc beta cells). In recent years, rapid progress has been made in the generation of sc-β cells and the establishment of pancreatic islet organoid models.
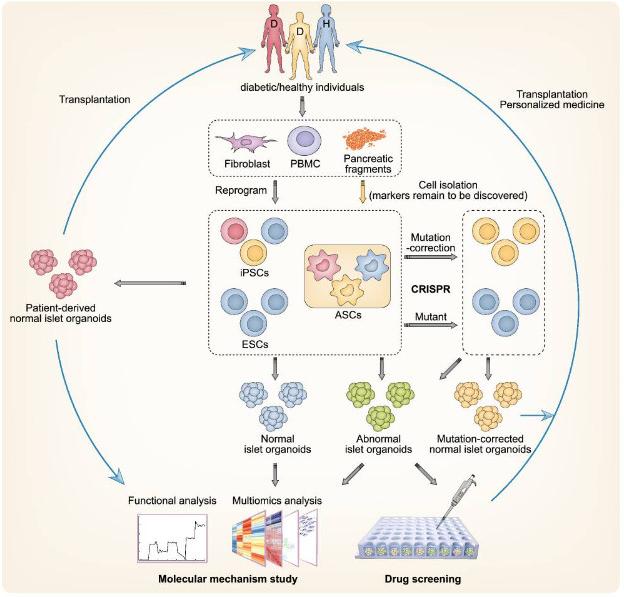 Figure 1 Promising applications of islet organoids in disease modeling and personalized medicine.1
Figure 1 Promising applications of islet organoids in disease modeling and personalized medicine.1
Strategies to Establish 3D Islet Organoids
Suspension-Based 3D Culture
The self-organizing ability of hPSCs has been widely used to aggregate dissociated hPSCs into 3D embryonic bodies (EBs), whose diameter depends on the culture system. Microfluidic devices provide a complex suspension-based strategy. Microfluidic perfusable systems continuously transmit induction signals or nutrients while clearing metabolic waste. In addition, perfusion can apply mechanical cues, such as flow induced shear stress related to physiology. Compared with the products obtained under static culture conditions, the pancreatic islet organoids produced by the perfusable system improved cell survival rate and cell acitvity, enhanced expression of mature endocrine cell markers, and significantly improved pancreatic islet function.
3D Culture Based on Suspension
Other strategies do not rely on self-organization to establish 3D structures, but instead use ECM components as scaffolds to promote 3D structure formation and cell matrix interactions. Isolated mouse embryonic pancreatic progenitor cells can survive in 2D culture, but organoids can only form in Matrigel, highlighting the role of cell matrix interactions in regulating cell fate. The 3D pancreatic islet organoid constructed within a scaffold combining collagen and Matrigel (C-M scaffold) produced alpha, beta, gamma, and PP cells. β-like cells express elevated levels of INS, GLUT2, and MAFA, and contain more than 12 times more insulin granules than cells cultured in 2D. In addition to promoting late maturation of endothelial cells, C-M scaffolds also provide a favorable microenvironment for endocrine commitment during early development, as evidenced by reduced expression of HNF6 (limited to exocrine cells of the natural pancreas) in 3D pancreatic progenitor cells compared to their planar counterparts.
Islet Organoids Models for Disease Research
Islet organoids provide a unique platform to investigate the complex cellular and molecular events that lead to β-cell dysfunction and destruction in diabetes.
Type 1 Diabetes (T1D)
Organoids can be generated from iPSCs of T1D patients and can recapitulate features of the disease, such as impaired insulin secretion and increased vulnerability to autoimmune attack. By co-culturing these organoids with immune cells from T1D patients, researchers can precisely dissect the mechanisms of β-cell destruction by autoreactive T cells and identify novel therapeutic targets to preserve β-cell mass or modulate the autoimmune response.
Type 2 Diabetes (T2D)
T2D is characterized by a combination of insulin resistance and progressive β-cell dysfunction. Organoids derived from T2D patient iPSCs can display impaired GSIS, reduced β-cell mass, and altered gene expression profiles associated with metabolic stress and inflammation. These models allow researchers to study the effects of chronic hyperglycemia, hyperlipidemia, and inflammatory cytokines on β-cell health and function.
Islet Organoids Models for For Drug Screening
The islet like organ is a better platform than other drug screening models for diabetes. With the advancement of iPSC technology and personalized medicine, patient derived beta cells and pancreatic islet organoids can serve as informative disease models, summarizing the pathogenesis and phenotype of specific patients, and can be used to evaluate patient specific drug responses after screening. In a proof-of-concept experiment to evaluate the possible application of drug screening, the sc - β cells of hiPSCs from T1D patients treated with three anti diabetes compounds showed increased insulin release. In addition, 4PBA successfully restored glucose responsiveness in pancreatic islet organoids of patients with Wolfram syndrome. However, the limited functionality and reproducibility of established pancreatic islet organoids need to be validated in other systems.
Frequently Asked Questions
Q: What are the current challenges facing the development and application of pancreatic islet organoids?
A: There are many challenges to overcome. The maturation and functional robustness of beta cells in organoids is a key issue. The replication of the natural vascular and neural innervation environment found in the pancreas is also crucial for long-term survival and function, especially for transplantation applications. The scalability of high-throughput drug screening and therapeutic production is another factor that needs to be considered. In addition, there is currently no standardized and widely accepted protocol for the generation of pancreatic islet organoids, which may lead to differences between studies.
Q: What are the potential clinical applications of pancreatic islet organoids?
A: Widely used in clinical practice. Pancreatic islet organoids can be used for autologous islet transplantation in T1D patients, and may not require lifelong immunosuppression, as patient specific iPSCs can be used to produce islets. Pancreatic islet organoids provide an unlimited source of insulin producing cells for cell replacement therapy. In addition, they are powerful tools for drug discovery and personalized medicine, capable of high-throughput screening of new therapeutic compounds and predicting individual patient responses to drugs in an in vitro system closely mimicking the natural environment.
Transform Your Research Using Parkinson's Disease Organoid Model from Creative Biolabs
Creative Biolabs is a 3D biology and organoid company focused on providing the highest-quality products and expertise to advance biomedical research and therapies. We are a leading custom research services provider offering an integrated portfolio of services based on our powerful 3D organoid platform. Our capabilities include services and products across the workflow, starting with cell source selection through disease modeling and high-throughput screening. Contact us today to learn more!
Organoid Models
Organoids Related Products
Research Model
Related Sections:

 Figure 1 Promising applications of islet organoids in disease modeling and personalized medicine.1
Figure 1 Promising applications of islet organoids in disease modeling and personalized medicine.1