Chimeric antigen receptor (CAR)-T cell therapy has achieved great clinical success. However, its wide application in various cancer types still faces major challenges, including insufficient efficacy due to the highly complex tumor microenvironment, and high costs due to personalized manufacturing procedures. To overcome these obstacles, many efforts have been made, focusing on optimizing chimeric antigen receptors, engineering and improving T cell capabilities, using the characteristics of T cells or NK cell subsets, or preparing ready-made universal T cells. In addition, since the advent of chimeric antigen receptor (CAR) technology, the clinical success of CAR-T cells has promoted new efforts to use CAR technology to generate CAR engineered immune cells from pluripotent stem cells.
The production of immune cells from human pluripotent stem cells (embryonic stem cells and induced pluripotent stem cells) has attracted attention in regenerative medicine. Immune cells derived from pluripotent stem cells, such as natural killer cells, macrophages, and lymphoid cells, especially T cells, can be used in immune cell therapy to treat incurable cancers.
At Creative Biolabs, we have developed a technology platform to produce immune cells derived from stem cells that express CAR. This technology platform for the first time provides an unlimited source of engineered stem cell-derived CAR-T/NK/MA immune cells, which can be used to eliminate cancer cells or regulate the tumor microenvironment in liquid and solid tumor immunotherapy. The engineering of CAR immune cells derived from pluripotent stem cells pave a new way for developing next-generation immune cell therapy.
Since human iPS cells can be reintroduced into patients through autologous transplantation without causing serious immune rejection, there is a strong interest in using iPS cells to generate therapeutic cells (such as hematopoietic stem cells, retinal pigment epithelial cells, and pancreatic β cells). Human pluripotent stem cells can differentiate into immune cells through cytokines and stromal cells, such as macrophages, natural killer (NK) cells, and T cells (Figure 1). Such derived immune cells can be used to treat tumors that cannot be cured by conventional clinical therapies (such as chemotherapy and radiation therapy).
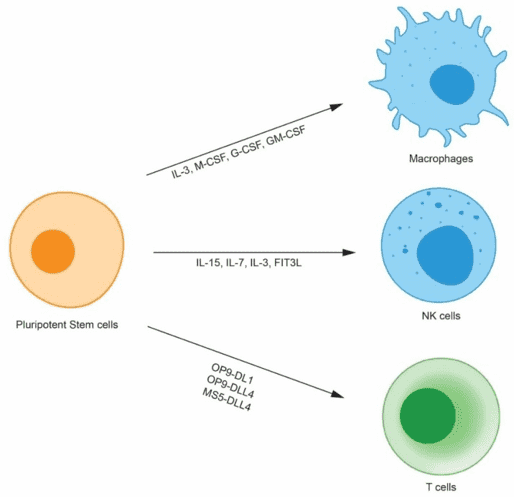 Fig.1 Human pluripotent stem cell-derived immune cells.1
Fig.1 Human pluripotent stem cell-derived immune cells.1
Since human pluripotent stem cells proliferate indefinitely, clonal selection can be performed after genetic modification, and an unlimited number of modified immune cells can be provided. Creative Biolabs is proud to present a powerful platform combing CAR cell therapy with the CRISPR/Cas9 technology to our worldwide clients, aiming to push their projects closer to clinical trials. By deploying CAR and CRISPR/Cas9 technology, human pluripotent stem cells can be engineered to knock out genes related to immune rejection, cytokine release syndrome, or express fourth-generation CARs, which can be used for precise anti-tumor activity and safety. The engineered stem cells-derived CAR cells can be cloned, selected, and expanded. This method can generate the next generation of immune cells, paving the way for the development of immune cell therapies, increasing efficacy, increasing cost-effectiveness, and improving the accuracy of anti-tumor activity.
For detailed information, please feel free to contact. Our team will get back to you as soon as possible.
Reference
For any technical issues or product/service related questions, please leave your information below. Our team will contact you soon.
All products and services are For Research Use Only and CANNOT be used in the treatment or diagnosis of disease.
 NEWSLETTER
NEWSLETTER
The latest newsletter to introduce the latest breaking information, our site updates, field and other scientific news, important events, and insights from industry leaders
LEARN MORE NEWSLETTER NEW SOLUTION
NEW SOLUTION
CellRapeutics™ In Vivo Cell Engineering: One-stop in vivo T/B/NK cell and macrophage engineering services covering vectors construction to function verification.
LEARN MORE SOLUTION NOVEL TECHNOLOGY
NOVEL TECHNOLOGY
Silence™ CAR-T Cell: A novel platform to enhance CAR-T cell immunotherapy by combining RNAi technology to suppress genes that may impede CAR functionality.
LEARN MORE NOVEL TECHNOLOGY NEW SOLUTION
NEW SOLUTION
Canine CAR-T Therapy Development: From early target discovery, CAR design and construction, cell culture, and transfection, to in vitro and in vivo function validation.
LEARN MORE SOLUTION